Products are selected by our editors, we may earn commission from links on this page.
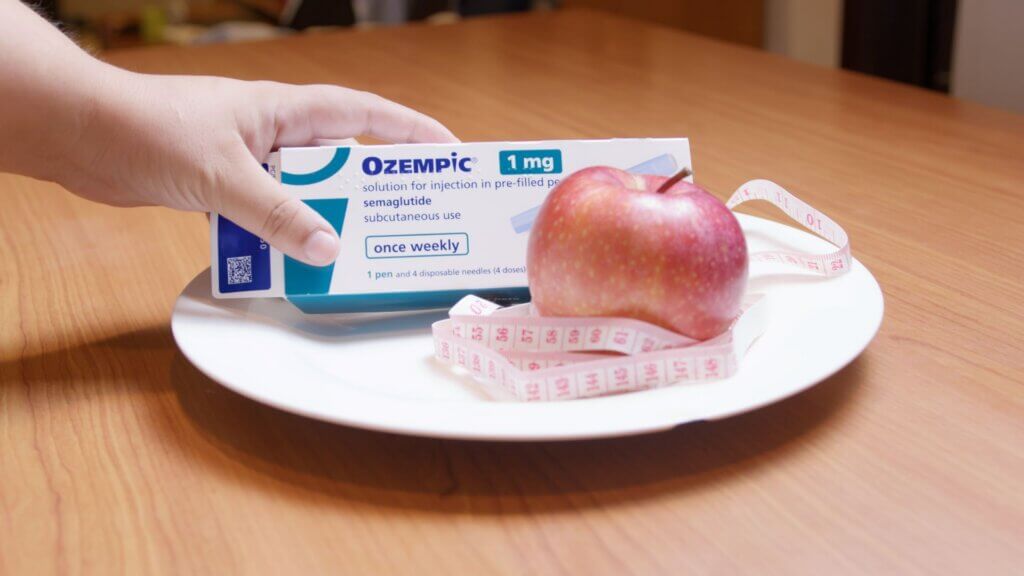
A disease historically associated with sailors who went weeks without vitamin-rich food during long voyages at sea is now emerging as an unexpected risk of modern weight-loss medications, according to researchers in Australia. Dietitians are sounding the alarm over GLP-1 drugs like Ozempic and Wegovy, warning that severe nutritional deficiencies can develop when patients eat too little or reach for the wrong foods while on the medication.
The Same Mechanism That Drives Weight Loss Is Creating a New Risk

GLP-1 and GIP medications drive weight loss by significantly reducing appetite and the sense of fullness. But Clare Collins, a laureate professor of nutrition and dietetics at the University of Newcastle in Australia, warns that this appetite suppression creates a gap between calories consumed and the full range of nutrients the body still needs, particularly when patients aren’t making deliberate choices about what they eat.
Decades of Trials Never Tracked What Patients Were Eating

A systematic review by the Hunter Medical Research Institute in Australia examined 41 clinical trials spanning 17 years and more than 50,000 participants. Only two of those studies recorded what patients were consuming while on GLP-1 medications. Collins wrote that nutrition is “largely missing from the evidence,” leaving a significant blind spot in how these drugs’ full health effects are understood.
Studies Reveal How Common Malnutrition Is Among GLP-1 Users

A 2025 study of adults with type 2 diabetes found that more than 20 percent developed nutritional deficiencies after 12 months on GLP-1 medications. A separate study of patients preparing for joint surgery found that 38 percent of GLP-1 users suffered from malnutrition, compared to just 8 percent among non-users.
A Famous Case Put Scurvy Back in the Headlines

British pop singer Robbie Williams told The Mirror last year that he had developed what he described as a “17th-century pirate disease” after taking a drug similar to Ozempic. That disease was scurvy, a serious vitamin C deficiency once common among sailors deprived of fruits and vegetables for months. “I’d stopped eating, and I wasn’t getting nutrients,” Williams said.
Scurvy’s Symptoms Are Severe and Often Missed Early On

Scurvy develops when the body is deprived of vitamin C over an extended period. According to the Cleveland Clinic, symptoms include anemia, loose teeth, bleeding gums, bruising, rough skin, swollen legs, and wounds that refuse to heal. In the worst cases, the disease can be fatal. Collins noted that for GLP-1 users already dealing with nausea and reduced appetite, early warning signs can be easy to overlook.
Scurvy Is Only One of Several Deficiency Risks Tied to GLP-1 Use

Vitamin C isn’t the only nutrient at stake. Collins noted that GLP-1 use has also been tied to thiamine deficiency, which can cause beriberi, a disease affecting the nerves and heart, or Wernicke’s encephalopathy, a potentially life-threatening brain disorder. She also flagged iron deficiency as a concern, noting it can cause anemia, a separate but equally real consequence for patients whose overall intake has dropped significantly.
Many Users Are Treating the Drug as Permission to Stop Eating

Los Angeles-based registered dietitian nutritionist Ilana Muhlstein says a troubling pattern has emerged: many GLP-1 users treat the medication as permission to severely restrict food without improving what they eat. “When your appetite is already low, and you’re experiencing nausea, the last thing you want to eat is salmon or vegetables,” she told Fox News Digital. “For these people, the risk of deficiency seems inevitable.”
Experts Are Laying Out a Clear Path Forward for Patients

Dr. Philip Rabito, an endocrinologist and weight-loss specialist in New York City, recommends screening all GLP-1 patients for nutrient deficiencies before starting treatment. For those who have significantly lost their appetite, Muhlstein advises supplementing with protein powder, fiber, omega-3s, and a quality multivitamin, while committing to structured sit-down meals. She also recommends that patients have labs drawn at least once a year to check vitamin and mineral levels.
Researchers Want Nutrition Built Into GLP-1 Care From Day One
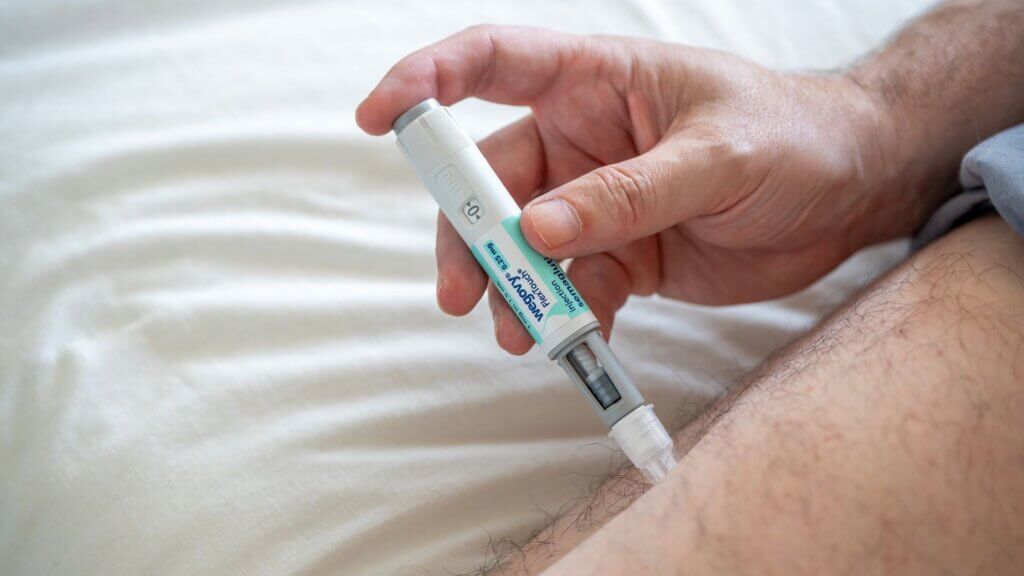
Collins is pushing for systemic change before cases like Williams’ become commonplace. “Let’s not wait for every GP to see a case of scurvy,” she said, calling for GLP-1 prescriptions to be automatically paired with dietitian referrals. Magriet Raxworthy, CEO of Dietitians Australia, added that without personalized medical nutrition therapy, patients remain at risk of muscle loss, bone density loss, and disordered eating that medication alone cannot address.
