Products are selected by our editors, we may earn commission from links on this page.

Doctors are urging caution after a Louisiana man spent four years misdiagnosed with schizophrenia, when in fact his terrifying hallucinations were caused by a prescribed pain medication. The case, published in the medical journal Cureus, underscores how opioid side effects can mimic psychiatric illness and why physicians must carefully evaluate sudden mental health symptoms in older patients.
Patient Background

The patient, a 67-year-old man from Louisiana, had a complex medical history that included coronary artery disease, high blood pressure, chronic back pain, and hepatitis C. He smoked cigarettes, occasionally used cannabis, but had no family history of mental illness, a fact that should have raised early diagnostic questions.
Initial Trigger at Age 63

At 63, he was hospitalized after suffering a seizure. Just three weeks later, he began experiencing vivid hallucinations. He described people breaking into his home, seeing bizarre animals, and feeling watched. Doctors diagnosed him with schizophrenia, despite the unusual late onset of symptoms.
Antipsychotic Treatment Begins
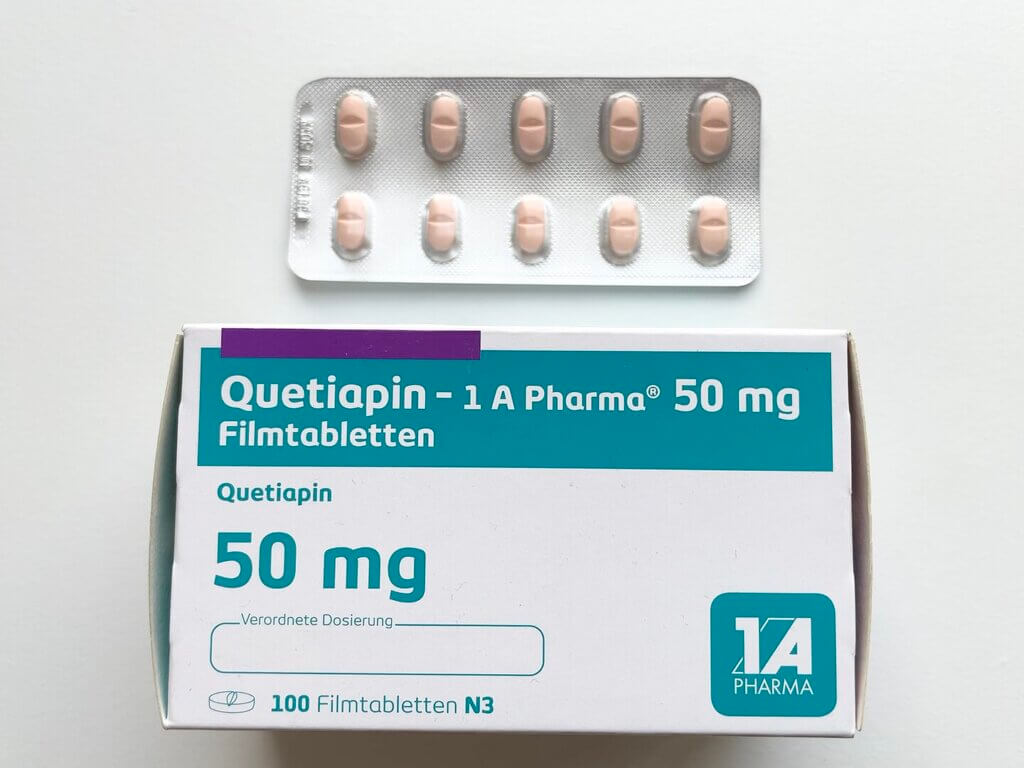
He was prescribed Quetiapine, an antipsychotic that helped him manage both the hallucinations and his sleep. For a time, his symptoms appeared to stabilize under psychiatric treatment.
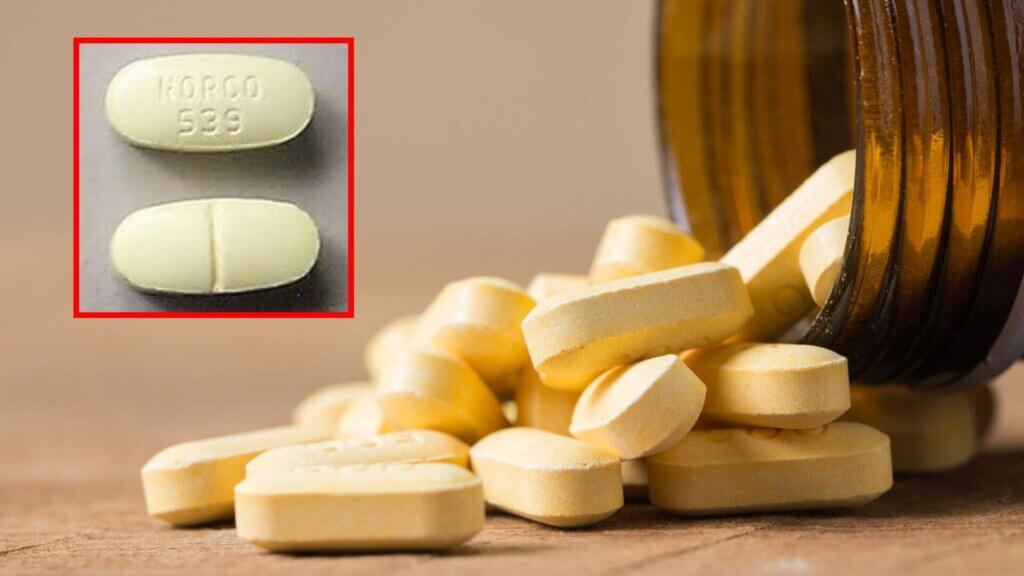
Norco Prescribed for Back Pain
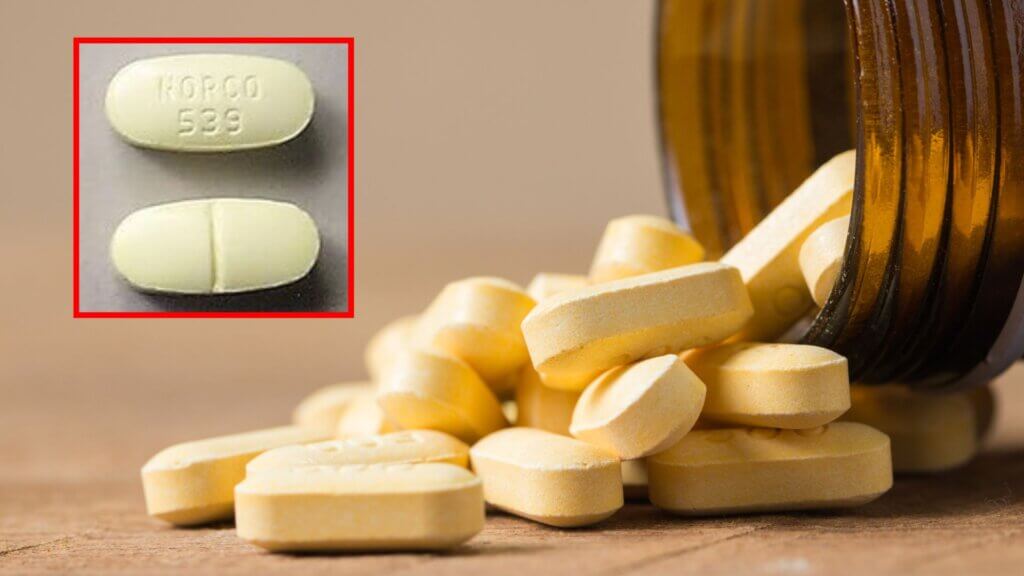
As his chronic back pain worsened, he was prescribed Norco (hydrocodone and acetaminophen). Initially, it eased his pain. But as his dosage was gradually increased, still within prescribed limits, his hallucinations escalated.
Hallucinations Intensify

The patient began reporting increasingly disturbing visions: worms crawling on the ceiling, people following him, and a growing sense of paranoia. These frightening episodes were initially attributed to his supposed schizophrenia, delaying recognition of the real cause.
The Patient Connects the Dots

Crucially, the man noticed a pattern himself—the more Norco he took, the more intense his hallucinations became. When he stopped taking the drug, the hallucinations disappeared entirely. This discovery was the turning point.
Doctors Reevaluate the Case

After reviewing his history, doctors concluded he did not have schizophrenia at all. Instead, he was suffering from opioid-induced hallucinations. His age, lack of family history, and the direct correlation with Norco use all pointed to medication, not mental illness, as the true culprit.
Clinical Lessons Learned
The case highlights a critical warning for physicians: in older adults, new-onset hallucinations should prompt suspicion of drug-induced neurotoxicity or other medical causes before psychiatric diagnoses are made. Misattributing such symptoms can lead to years of unnecessary treatment and suffering.
A Misdiagnosis With Lasting Consequences

This Louisiana man’s ordeal serves as a sobering reminder that not all hallucinations are psychiatric. Commonly prescribed medications, even at normal doses, can produce severe neurotoxic effects. Both patients and doctors are urged to watch for new psychiatric symptoms following a medication change, as recognizing the cause early could prevent years of misdiagnosis.